Home Care Collective: A Case Study in Architecting Senior Support in Japan
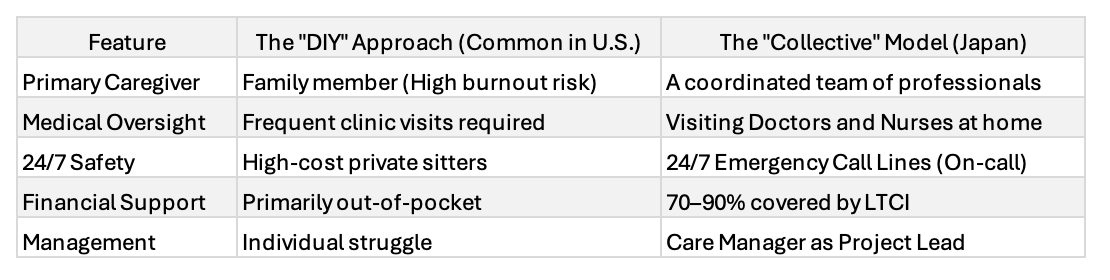
In the U.S., Aging in Place is often a DIY project. In Japan, it is a national strategy designed to keep you in your home for as long as humanly possible.
But let’s be clear: Home is not a hospital. While Japan’s infrastructure allows us to build a robust support team, there is a reality where 24/7 care at home reaches its limit.
The " Home Care Collective " is designed to delay the facility, but it’s just as important to know when to call a tactical retreat.
Quick Summary
Table of contents
1. 2026 Reality: Why Home Care Collective is Necessary
2. Human Infrastructure
3. Sample Daily Schedule (Care Level 1)
4. When the Collective Reaches Its Limit: Red Flags
5. Strategy: Do Not Quit Your Job to Become a Full-Time Caregiver
6. Tough Reality: What to Watch Out For
7. Wrap-up: Risk Management for Your Future
1.2026 Reality: Why Home Care Collective is Necessary
According to the Ministry of Health, Labor and Welfare, nearly 20.1% of those aged 65 and over now require some level of certified care. However, the "Helper" shortage is real. In 2026, we are seeing high turnover and agencies struggling to fill shifts.
You cannot simply buy care and walk away. You must become the manager of a multi-disciplinary team.
Real story
In 2022, my father’s life changed in an instant when he fell off his bicycle, triggering a decline in his mobility due to spinal stenosis. Like many seniors, he refused to move into a care facility. To honor his wish to stay at home, we had to build what I call the Home Care Collective.
Related article
In-Home Care in Japan: From Critical Illness to Senior Support
Senior Care in Japan: Costs, Choices, and What Foreigners Should Know
2.Human Infrastructure
A resilient home care model requires a mix of medical, physical, and logistical support. Here is the breakdown of my father’s Home Care Collective:
1.Visiting Doctor (Zaitaku-i)
Most Japanese cities now have robust networks of doctors specializing in home visits. Depending on the patient's stability, they typically visit 1–2 times per month to manage chronic conditions and prescriptions. This system transforms the home into a clinical space, allowing seniors to receive professional medical oversight without the physical strain of traveling to a clinic.
2. Visiting Nurse (Houmon Kango)
The visiting nurse acts as the medical “eyes and ears” of your care team. Under Long-Term Care Insurance (LTCI), the frequency of visits varies depending on the individual’s condition—from once a month to daily—to monitor vital signs and manage pain.
One of the most valuable features is the 24/7 emergency call line, which provides significant peace of mind for family members living at a distance. Information from each visit is shared with the attending physician and care manager, ensuring coordinated care.
Your Challenge: A 24/7 call line is only effective if the senior can actually use it. In many cases, hearing impairment and frailty made it difficult for seniors to reach or respond to the phone. You need to actively assess this safety net and confirm that your loved one can realistically trigger help when needed.
Personally, I recommend using a commercial emergency alert device worn around the neck, which allows seniors to call for help with a simple press of a button.
3. Home Helpers (Houmon Kaigo)
These are the "boots on the ground" for daily life. Depending on the assigned care level, they manage essential tasks like garbage disposal, light cleaning, grocery shopping, and hygiene support (including diaper changes and feeding for higher care levels).
Understand boundary: It is important to remember that helpers are restricted from providing medical treatment. Even seemingly simple tasks, like administering medication, are subject to strict regulations.
Furthermore, because helpers are employees of an agency—not your personal employees—they cannot perform tasks outside the pre-approved Care Plan. They are also not contractually obligated to provide status reports to the family; their primary duty is the execution of the plan itself.
4. The Care Manager (CM)
If the Home Care Collective is the team, the Care Manager is the Project Lead. This is the most critical relationship in the Japanese system.
Based on the assigned care level, your CM evaluates seniors needs and build the actual service schedule and serves as your primary contact for adjusting care levels or addressing new challenges. They typically visit the home monthly to assess the situation and chair a full team review meeting—usually twice a year—which requires family participation.
Advice for Foreign Residents: Chemistry is critical. If you feel your CM doesn’t understand your unique needs of an international family or lacks initiative, remember that you have the right to request a change. Do not settle for a manager who isn't a partner in your strategy.
5. Specialized Support & Equipment
The Collective is supported by a network of specialized vendors who bridge the gap between medical care and daily living:
Rehabilitation: Professional therapists visit the home to provide massage and mobility exercises. These services are typically covered under the Long-Term Care Insurance (LTCI) plan and are essential for maintaining physical independence.
Meal Delivery Services: Daily delivery of nutritionally balanced meal boxes ensures consistent calorie intake and removes the physical burden of cooking or grocery shopping.
Assistive Equipment Suppliers: This includes the rental of specialized beds, walkers, and the installation of safety features like handrails. Notably, these equipment providers are active participants in the semi-annual team review meetings, ensuring the home environment evolves with the senior's needs.
Medical Taxi Services: Specialized transportation for clinic visits that often includes "door-to-doctor" accompaniment. This is a critical service for family members who cannot personally escort seniors to every appointment.
The Evolving Workforce: Due to domestic labor shortages, many care workers now come from Southeast Asia (Philippines, Indonesia, and Vietnam). Many of these professionals speak English, and utilizing translation technology like VeuvoDisplay can bridge communication gap.
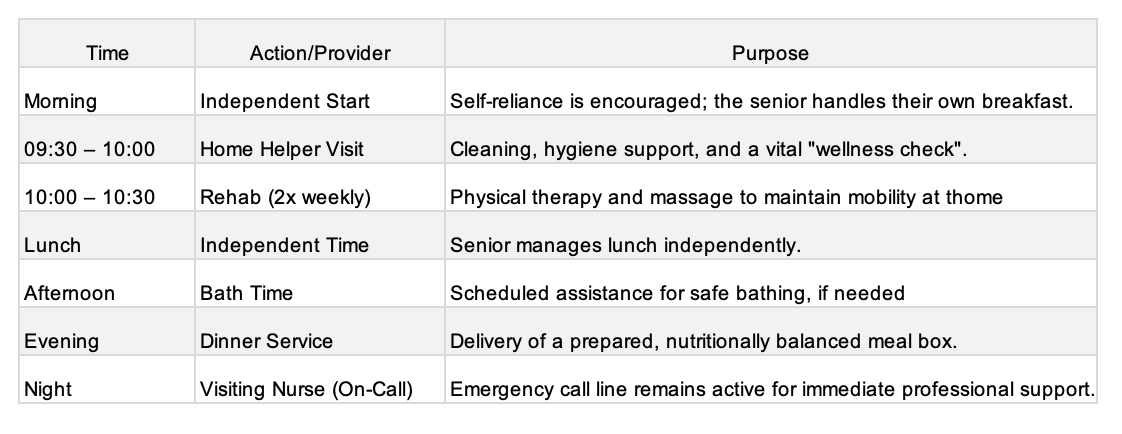
3. Sample Daily Schedule (Care Level 1)
What does 24/7 support actually look like? It is rarely one person staying in the house for 24 hours. Instead, it is a relay of professional services.
The following schedule is a real-world example for a senior at Care Level 1. In this case, the individual maintains some mobility with a walker and can manage daily activities inside the home—even walking to the mailbox for the daily newspaper.
Navigator Tip: Limits of the Relay
This "relay" model is designed to maximize a senior's autonomy while ensuring professional contact at key intervals. However, technology and professional services are only part of the equation.
Human Gap: While the Home Care Collective handles daily logistics, family involvement remains essential for high-level advocacy—such as attending doctor’s consultations, managing complex banking, or filing tax returns.
Nutrition Gap: Meal delivery services are efficient and nutritionally balanced for seniors, but they often lack the variety and warmth of a home-cooked meal. In my experience, while these services provide the necessary calories, a family’s home-cooked meal provides the “spirit.”
4. When the Collective Reaches Its Limit: Red Flags
You must identify when home care transitions from "support" to "unsafe." While helpers monitor daily tasks, family observation are often the first to see the subtle alarms of systemic failure.
Sleep Gap: If a senior needs repositioning or hygiene every two hours at night, it is time to increase care level. Night-visit care exists, but it is municipal-dependent.
Medical Complexity: When care shifts from social support to clinical management—like ventilator settings or severe organ dysfunction—a specialized facility or hospital becomes the safer, more logical choice.
Cognitive Safety: Severe dementia involving wandering or fire risks requires the closed security of a memory care facility that a standard home cannot provide.
Real Story: Fading Safety Net
Initially, my father could manage a phone. As his hearing declined, that safety net became shaky. I also noticed he had short breathring occasionally, which triggered the move toward a higher care-level evaluation.
Roadmap: Senior Care Level 5
Japanese system scales from Level 1 to 5. Level 5 is the "Full Support" stage and usually the final signal to transition to a facility:
Total Assistance: Required for every movement (eating, bathing, toileting).
Bedridden: The senior spends the majority of their time in bed.
Mental Capacity: Heavy dementia or stroke effects make meaningful interaction difficult.
Practical Solutions: The Strategic Transition
Bringing up a facility move is emotionally fraught, but your Home Care Collective makes this transition smoother. You aren't making a blind choice in a crisis; you are leveraging a team that already understands the senior’s history and personality to find the right destination.
5.Strategy: Do Not Quit Your Job to Become a Full-Time Caregiver
As a former HR professional, my strongest advice is this: Do not resign from your career to become a full-time caregiver.
In Japan, roughly 100,000 people leave the workforce each year to provide family care.This often leads to a triple crisis: financial ruin, severe caregiver burnout, and immense difficulty re-entering the workforce later.
Leveraging Corporate Support
Under Japanese Labor Law, you are entitled to specific benefits to help you set up your support system. These are separate from your annual paid leave (Paid Time Off). Paid or unapid depends on the company rule.
Family Care Leave (Kaigo Kyuka): Up to 5 days per year (per family member) for immediate tasks like doctor visits.
Family Care Leave (Kaigo Kyugyo): Up to 93 days total (which can be split into three separate periods). During this time, you may be eligible for a government benefit covering approximately 67% of your salary.
Flexibility Benefits: Many companies offer reduced working hours, flextime, telecommuting (Work From Home), and exemptions from overtime to accommodate caregiving
Real Story 1: The Speed of the System
When my father was hospitalized after a fall, I immediately told the assigned Care Manager I was managing this from a distance. The team moved with incredible speed: by the day he was discharged, the Care Manager had already evaluated his needs, moved all necessary equipment into the house, and scheduled a helper for the next morning. The system works fast when you communicate your professional boundaries early.
Real Story 2: Managing the Leave Hurdle
Many employees hesitate to take Family Care Leave, fearing it will hurt their career. However, I have seen employees use this time specifically to "architect" their Home Care Collective.
One colleague used their leave to stabilize the support team and then returned to work using a mix of telecommuting and reduced hours. By being transparent with their team and expressing gratitude, they maintained their career while the Collective handled the daily care.
6. Tough Reality of 2026: What to Watch Out For
We must be honest about the structural challenges of this model. Success requires acknowledging these four variables:
Geographic Divide: In rural Japan, caregiving is a pillar of the local economy; as a result, staffing is often more stable and consistent.
In major cities like Tokyo, competition for labor is fierce, making it harder to secure steady home care. However, urban areas offer a distinct advantage for international families: significantly better English-language support and more globalized medical resources.
Communication Gap: As cognitive decline progresses, simple tasks become impossible. We solved this by introducing web cameras and specialized tools to monitor safety and facilitate communication remotely.
Frozen Account Risk: Once a senior loses mental capacity, their bank accounts may be frozen by the bank. While we secured a proxy card early, formal legal guardianship or trusts must be discussed before a crisis occurs.
See also: Will Your Accounts Freeze? Navigating Cognitive Decline & Banking in Japan [2026 Guide]
Navigator’s Summary Checklist
[ ] Identify your Care Manager: Treat this person as your most important strategic partner.
[ ] Map the Home Care Collective: Build a diversified team of doctors, nurses, and rehab staff—do not rely on a single helper.
[ ] Secure Digital Access: Set up LINE, Zoom, or web cameras for remote monitoring before mobility declines.
[ ] Establish Financial Proxies: Secure bank proxy cards and discuss legal guardianship while mental capacity is still clear.
7.Wrap-up: Risk Management for Your Future
My father chose to stay at home. Despite his physical limitations, he finds joy in his independence and his own space. But this dignity is only possible because we built the logistical infrastructure before the crisis peaked.
Senior care in Japan is "ten people, ten colors"—every situation is unique. However, the rule of management remains the same: start early. Ensure your emergency routes are clear, your Care Manager relationship is strong, and your financial proxies are in place.
Aki | Japanese | Former Head of HR in Global Finance
Aki has served as Head of Human Resources in the global financial sector. With over two decades of experience navigating labor law, residency, and wealth protection in both Tokyo and Chicago, she now provides the "insider’s roadmap" for foreigners planning a stable, high-value long-term life and retirement in Japan.
Referrals
Official Caregiving Support Guidelines & System Overview (MHLW Japan – PDF)
Caregiver Leave System in Japan (Ministry of Health, Labour and Welfare)
Short-Term Care Leave (Family Care Leave) Explained – Japan MHLW Guide
Official Guide to Balancing Work and Caregiving (PDF – MHLW Japan)